Abstract:
The big question for every physician or healthcare provider is how to survive, or rather thrive, in the uncertainty of today’s healthcare environment. This article is not intended to answer questions about mergers with other practices or purchases by hospitals and other entities. Instead, this article intends to encourage a look at the basic business model of your practice environment using the SWOT approach: Strengths, Weaknesses, Opportunities, and Threats. We review some of the basic questions and explore some possible answers. We look at your business, and discuss aspects that we believe are key to long-term survival for your practice.
Regardless of your clinical specialty, it is important to consider what you are offering to the patients who seek care in your practice.
The place to start is with the patient. It is likely that any provider, while seeing patients in the office on any given day, will see one of four different types of patients:
The patient seeking diagnosis or basic treatment: The patient’s condition could be as simple as a cold, or as complex as a serious heart ailment. In some cases immediate treatment is provided and the issue is resolved. In other cases, the need for a care plan—acute or chronic in nature—will complete that day’s visit.
The patient who has been diagnosed and is in need of more advanced treatment: In some cases, this treatment may occur in the office, but mostly it is given in other, more appropriate settings.
The chronic patient who has been seen before, perhaps many times, in the office or other settings: This would apply to patients with diabetes, obesity, heart, kidney, or other chronic conditions.
The patient seeking a wellness exam: This would encompass patients in need of preventive services including annual wellness exams.
In meeting the need for population health, all providers, regardless of specialty or training, have a role to play in addressing patient expectations and population need.
As a provider, are you meeting the needs and providing the best treatment option for that patient in your office setting? If the practice is so busy that you have only a few minutes with each patient, are you using your resources effectively? Should you even be seeing the patient for that level of care in that setting? Do you have the resources available in your setting to provide optimal care to the patient? Can you get reimbursed appropriately for meeting that patient’s need?
Before we go any further, consider the payment models noted in the continuum framework. It may be that the diagnostic visit is fee-for-service; the treatment visit could be part of a bundled package; the chronic visit might be part of a capitation model; and the wellness visit could belong to any of those three options. Are your treatment plans geared around payment options? Do you treat patients differently if they are fee-for-service versus one of the other options? If so, why? Are financial incentives driving these decisions, or are you offering the best possible option for care?
Let’s look at each of the different patient phases by asking additional questions:
For the patient in need of diagnosis may need an x-ray or lab service, do you have those capabilities in the office? If it is necessary to send out for service, is that cost effective? Is that best for the patient?
If you have a capitation contract, is it better to refer out, from a cost point of view, or should you purchase the appropriate equipment? Have you considered whether, even though it may not be a direct return on investment, it would be cheaper to provide the service in the office rather than refer out?
In the wellness exam, do you pre-order diagnostic procedures so you can review results, or do you make the patient come back for a “sickness” visit to review results?
This may seem like a lot of questions, but in order to honestly assess your practice, you need to perform a true detailed review of everything.
Let’s now look at your practice in greater detail. An honest assessment of how well you are doing—what is good and what is bad—is a great place to start. The long-proven format of a SWOT analysis helps to identify these factors. The SWOT analysis—which stands for Strengths, Weaknesses, Opportunities, and Threats—is a way to structure a review of what you consider to be your strengths and weaknesses internally as well as the opportunities and threats related to your position in the local market. It is critical to be honest and complete. Figures 1 through 4 will guide your review.

Figure 1. Strengths.

Figure 2. Internal weaknesses.
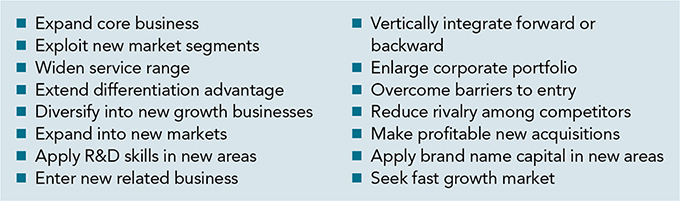
Figure 3. Environmental opportunities.

Figure 4. Environmental threats.
As we dive deeper into this honest assessment of your practice, the following key areas must be reviewed:
Organizational structure
Do you have the right legal arrangement to meet professional and taxation issues?
Should you join another group, sell, or take the lead in expansion?
Does your current organizational structure work? Is it divisional or departmental or location specific? Are controls, communication models, and decision-making levels defined, and do they work well?
Do you have a process in place for annual review?
Location
Is the current office location the best?
Are we meeting the needs of the patients that we serve?
Should we expand or contract our locations to optimize our efficiency or to best serve our patients?
Credentials
Is our paperwork up to date (e.g., licensure, DEA)
Do we have a structure in place to ensure nothing falls through the cracks and all required credentials are in place, regularly reviewed, and updated?
Do we have a system in place to effectively add a new provider?
Do we have a process in place for annual review?
Accounting and reporting
Does the existing financial accounting and reporting system work?
Do we have checks and balances in place?
Do we get the information we need in a timely fashion to allow for decision making and effective communication to all owners?
Is staffing adequate, well trained, and effective in communication?
Does the budget development, reporting, and updating process work?
Do we know, understand, and control costs?
Is the revenue cycle optimal?
Do we have a process in place for annual review?
Fee schedule
Is the current fee schedule appropriate for Medicare and all payer contracts?
Do we manage private payment options appropriately?
Do we review our schedule at least once annually?
Coding
Do we have the necessary resources available to answer any questions?
Do we review coding decisions and documentation regularly? How?
Do we track denials or other issues around coding?
Do we have a compliance system in place to address outliers?
Do we have a process in place for annual review?
Software
Do we have the right EMR and PMS systems? How effective is the interface?
Do we have appropriate maintenance agreements?
Do we have a cybersecurity system in place?
Do we receive adequate training and support from our vendor(s)?
Is there anything else required to interface with practice areas?
Do we have a process in place for annual review?
Communication
Do we have the right telephone system?
Does the answering service work?
Do we have adequate cell phone use, policy for use, and security in place?
Does the Internet work?
Do patients have access to the Internet in the reception area? Does that requirement affect staff use, and do we have a policy in place on access?
How effective is the patient portal?
Do we have a process in place for annual review?
Equipment and supplies
Do we have the right operational equipment?
Do we have the right ancillary equipment?
Do we have maintenance agreements?
How do we control inventory?
Do we have checks and balances for controls on ordering and inventory?
Do we have a process in place for annual review?
Marketing
How effective is our marketing program?
Do we use social media effectively?
Do we have an annual budget in place?
Are we serving the right population?
Do we have adequate reporting and analysis to ensure optimum market penetration?
Do we have a process in place for annual review?
Operations
Do our processes work?
Are scheduling, handling of new patients, and tracking follow-up visits effective?
What is our cycle time per provider and location?
What is the third new patient available slot per provider?
Does our interdepartmental transfer of patients and data work?
Do we have a process in place for annual review?
Insurance
Do we have adequate insurance to cover disaster, business loss, fire, cybersecurity, and the like?
Do we have the right agent(s)?
Do we have a process in place for annual review?
Human resources
What is our staffing ratio this year compared with last year?
Do we have the right metric to measure staffing levels?
Do we have an effective staff training program?
Do we have an appropriate benefit package? Is it well documented in the employee handbook?
Do we have an effective recruitment, selection, on-boarding, and retention process?
Do we have an effective discipline program?
Do we pay adequately?
Do we have a process in place for annual review?
Compliance/Quality
Does our compliance program work?
Does it cover all necessary areas to meet federal and state regulations?
Do we adequately monitor compliance with all internal policies and procedures?
Do we emphasize quality?
Do we have evidence-based treatment plans in place?
Do we monitor and manage internal and patient safety programs?
Do we have a process in place for annual review?
Let’s compare this honest assessment of the practice with something more familiar. The training of a physician includes not only looking at the patient’s condition, but also looking at the symptoms and then deeper to the etiology. We can apply the same approach when assessing a practice. When looking at the practice, we must consider the following:
Practice condition
Review of assessment checklist
What are the key performance indicators? (e.g., financial statement, turnover, patient visits)
What are the patient satisfaction scores?
Symptoms
Too busy
Not enough provider time
Low inventory
Things never in the right place
Crisis hire pattern
Etiology
Unclear mission
Confused or multiple cultures
Poor talent, staff hiring, and retention
This list is intended to start your thought process on how effective and efficient your practice currently is; it is by no means complete. The gaps that you discover should give you a roadmap to improvement.
Topics
Critical Appraisal Skills
Differentiation
Financial Management
Related
The Collaboration Imperative: Why Healthcare Executives Must Unite Against an Existential ThreatResuscitating Healthcare: 80 Years of Federal Laws, Financing, and Future ForecastImproving the Physician Experience to Attract, Retain, and Engage Top Physician Talent — Part 3: Rethinking Physician Development and Advancing from Competence to Continuous Improvement

